
Prospective cohort study of the treatment of non-neoplastic epithelial disorders of the vulva with a fractional Carbon Dioxide laser
Introduction
Non-neoplastic epithelial disorders of the vulva are a group of chronic lesions in which degeneration and pigment changes occur in the skin and mucosal tissues of the vulva. The main symptoms are pruritus or pain of the vulva, rough vulvar skin, hypopigmentation, chap, atrophy, adhesions, and even carcinogenesis, all of which seriously affect quality of life (1). Common pathological types of non-neoplastic epithelial disorders of the vulva include lichen simplex chronicus and lichen sclerosus. The number of women with non-neoplastic epithelial disorders of the vulva accounts for 0.05% to 1% of the total number of women. Perimenopausal women have a high prevalence of non-neoplastic epithelial disorders of the vulva. The average age at non-neoplastic epithelial disorders of the vulva onset is 52.6 years (2). However, in recent years, the incidence of non-neoplastic epithelial disorders of the vulva has had a clear upward trend, and during that time, the age of onset has become significantly younger.
The main purpose of clinical treatment of non-neoplastic epithelial disorders of the vulva is to relieve symptoms, prevent further development of symptoms, and improve the quality of daily life. Currently, there are a variety of methods to treat this disease, including medication (topical administration of vitamin A ointment or corticosteroid ointment, oral administration of vitamin E and vitamin A), cryotherapy, and electrostimulation of smooth muscle. These therapeutic methods have different efficacies. Therefore, selecting an appropriate and effective therapeutic method is very important for improving patient quality of life. Scientific evidence for clinical practice is urgently needed from comparisons of improvement in subjective symptoms and therapeutic efficacies of various therapeutic methods.
In recent years, fractional Carbon Dioxidelaser techniques have achieved good clinical results for the treatment of skin lesions. Mezzana et al. found that a fractional Carbon Dioxidelaser can significantly improve local skin microcirculation due to the thermal effects of micropores (3). However, there are few reports on the treatment of non-neoplastic epithelial disorders of the vulva using a fractional Carbon Dioxidelaser. Therefore, this study aimed to evaluate and comparatively analyse the therapeutic efficacies of the electrostimulation of smooth muscle and a fractional Carbon Dioxidelaser for treating non-neoplastic epithelial disorders of the vulva using the Patient Global Impression of Change (PGI-C) scale and a clinical efficacy rating scale 3, 6 and 12 months after completion of treatment. The therapeutic outcomes of the 2 therapeutic methods on 2 pathological subtypes, lichen simplex chronicus and lichen sclerosus, were compared to find a safer and more effective treatment for non-neoplastic epithelial disorders of the vulva and to guide clinical treatment decision-making. We present the following article in accordance with the STROBE reporting checklist (available at https://gpm.amegroups.com/article/view/10.21037/gpm-20-40/rc).
Methods
Study subjects
This study included 98 patients with lichen simplex chronicus or lichen sclerosus confirmed by vulvar biopsy at the West China Second University Hospital of Sichuan University from November 2016 to March 2018. All patients voluntarily participated in the study and signed an informed consent for clinical studies. Patients who met any of the following criteria were excluded: (I) pregnant patients or patients with recent fertility attempts; (II) patients with a history of photosensitivity; (III) patients with severe systemic internal diseases that have affected daily life (e.g., severe cardiovascular diseases and immune diseases); (IV) patients with psychological and psychiatric disorders, such as depression, who are unable to complete the follow-up; (V) patients who received other physical therapies within the recent 3 months; (VI) patients with atypical vulvar epithelial hyperplasia or vulvar cancer; (VII) patients with diabetes; (VIII) patients with other specific skin diseases; and (IX) patients with tumours and acute inflammation of the reproductive system. Finally, after excluding 18 patients who met the above exclusion criteria, a total of 80 patients (meeting the sample size requirements) were enrolled in the study. Patients were divided into 2 matched groups by age, pathological subtypes, and disease severity. One group was treated with electrostimulation of smooth muscle (the electrostimulation group), and the other group was treated with fractional Carbon Dioxide laser (the laser treatment group). Each group had 40 patients and included 20 cases of lichen simplex chronicus and 20 cases of lichen sclerosus. Baseline data of the patients are shown in Table 1. This study was approved by the ethics committee at West China Second University Hospital, Sichuan University (registration number: 2019YJ0044). The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). All patients voluntarily participated in the study and signed an informed consent for clinical studies.
Table 1
| General information | Electrostimulation group (N=40) | Laser treatment group (N=40) | Statistics | P | |||
|---|---|---|---|---|---|---|---|
| Mean | Standard deviation | Mean | Standard deviation | ||||
| Age | 41.43 | 11.98 | 44.89 | 11.52 | 0.35 | 0.946 | |
| BMI | 22.18 | 2.92 | 23.95 | 3.03 | 0.88 | 0.469 | |
| Disease course | 3.69 | 1.58 | 3.71 | 2.46 | 0.7 | 0.500 | |
| Pretreatment clinical score | 6.52 | 1.41 | 6.63 | 1.20 | 0.06 | 0.935 | |
BMI, body mass index.
Therapeutic method
Electrostimulation of smooth muscle
A PHENIX 8-PLUS abdominopelvic electrostimulation therapy device (Electronic Concept Lignon Innovation, France), which includes a lipid and smooth muscle electrostimulation component (ML-36) and an abdominopelvic electrostimulation therapy system was used to electro-stimulate smooth muscle. Each patient had 3 treatment courses, each treatment course included 10 treatments, and each treatment took 40 minutes. In the first treatment course, patients were treated once a day; in the second treatment course, patients were treated once every other day; and in the third treatment course, patients were treated 2–3 times per week.
Fractional Carbon Dioxide laser treatment
A multifunctional Carbon Dioxidelaser platform (Femilift, Alma Lasers, Israel) was used to treat patients for 1 treatment course, and each treatment course included 3 treatments. Patients were treated once every 4 weeks.
Clinical follow-up and efficacy evaluation indicators
The PGI-C scale (4) (see Table S1) and the clinical efficacy rating scale (5) (see Table S2) were used to evaluate the therapeutic efficacy of patients at follow-up 3, 6, and 12 months after the completion of treatment. The efficacy index was calculated as follows: efficacy index = (total pre-treatment score – total post-treatment score) / total pre-treatment score × 100% (6). Based on the calculated efficacy index, the treatment outcomes were divided into the following: cured (efficacy index ≥90%), effective (89% > efficacy index >21%), and ineffective (efficacy index ≤20%). Total effective rate (%) = (Number of cured cases + Number of effective cases) / Total number of cases × 100%.
Statistical methods
The software package SAS 9.3 was used for statistical analysis. Measurement data that conformed to a normal distribution was expressed as the mean ± standard deviation, and independent samples t-test or analysis of variance (ANOVA) was performed for intergroup comparison. Count data were statistically described using number of cases, rate, or ratio, and the chi-square test or Fisher’s exact test was performed for intergroup comparisons. P<0.05 indicated a statistically significant difference, and the significance level was a=0.05.
Results
Baseline data
The patients in the 2 groups had no significant differences in age, BMI, disease course, and disease severity (P>0.05). The detailed data are provided in Table 1.
Comparison of therapeutic efficacy
PGI-C scores
As shown in Table 2, the PGI-C scores for the laser treatment group and the electrostimulation group were significantly different at 3, 6 and 12 months after the completion of treatment (P<0.05 for all time points). The detailed data are provided in Figure 1. Among them, the subjective improvement in the laser treatment group was better than that in the electrostimulation group, and a high proportion of the patients in the laser treatment group achieved significant improvement in symptoms, reaching 65.00% (26/40) 3 months after the completion of treatment, whereas that of the electrostimulation group was 35.00% (14/40). Because the disease is prone to relapse, after the completion of treatment, the number of patients with significant improvement in symptoms gradually decreased over time in both groups. In the laser treatment group, 26, 22, and 20 patients indicated significant improvement in symptoms 3, 6 and 12 months, respectively, after the completion of treatment. In the electrostimulation group, 14, 12, and 10 patients indicated significant improvement in symptoms 3, 6 and 12 months, respectively, after the completion of treatment. Twelve months after the completion of treatment, the proportion of patients with significant improvement in subjective symptoms in the laser treatment group also decreased, but the effective rate still reached 50%.
Table 2
| PGI-C | Significantly improved | Improved | Slightly improved | Unimproved | Total | P |
|---|---|---|---|---|---|---|
| 3 months | ||||||
| Electrostimulation group | 14 | 12 | 9 | 5 | 40 | 0.035 |
| Laser treatment group | 26 | 9 | 4 | 1 | 40 | |
| 6 months | ||||||
| Electrostimulation group | 12 | 10 | 13 | 5 | 40 | 0.012 |
| Laser treatment group | 22 | 13 | 4 | 1 | 40 | |
| 12 months | ||||||
| Electrostimulation group | 10 | 10 | 15 | 5 | 40 | 0.008 |
| Laser treatment group | 20 | 14 | 5 | 1 | 40 |
Efficacy scores
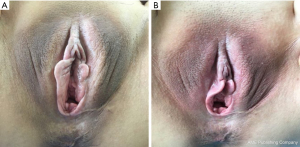
From the comparison of efficacy levels determined by efficacy scores 3 months, 6 months, and 12 months after the completion of treatment, the therapeutic efficacy of the laser treatment group was significantly different from that of the electrostimulation group (P<0.05 for all time points) (Table 3). As shown in (Table 4), the total effective rate for patients in the laser treatment group (90.00%) was higher than that for patients in the electrostimulation group (77.50%) 3 months after the completion of treatment; the total effective rates for the electrostimulation group decreased 3 and 6 months after the completion of treatment (72.50% and 67.50%, respectively). In the laser treatment group, although the total effective rates 6 months and 12 months after the completion of treatment was slightly lower (2.50%) than that 3 months after the completion of treatment, the total effective rate stabilized at 87.50% (Figures 2,3).
Table 3
| Clinical efficacy score | Before treatment | 3 months after treatment | 6 months after treatment | 12 months after treatment |
|---|---|---|---|---|
| Electrostimulation group (N=40) | 6.5±1.4 | 3.5±2.9 | 4.0±3.0 | 4.3±3.5 |
| Laser treatment group (N=40) | 6.6±1.2 | 2.5±2.2 | 2.1±2.0 | 2.1±2.0 |
Table 4
| Efficacy score | Cured | Effective | Ineffective | Total effective rate | Total | P |
|---|---|---|---|---|---|---|
| 3 months | ||||||
| Electrostimulation group | 1 | 30 | 9 | 77.50% | 40 | 0.410 |
| Laser treatment group | 2 | 34 | 4 | 90.00% | 40 | |
| 6 months | ||||||
| Electrostimulation group | 1 | 28 | 11 | 72.50% | 40 | 0.260 |
| Laser treatment group | 2 | 33 | 5 | 87.50% | 40 | |
| 12 months | ||||||
| Electrostimulation group | 1 | 26 | 13 | 67.50% | 40 | 0.070 |
| Laser treatment group | 2 | 33 | 5 | 87.50% | 40 |

Comparison of the therapeutic efficacy for pathological subtypes
PGI-C scores
The laser treatment group and the electrostimulation group each included 20 cases of lichen simplex chronicus and 20 cases of lichen sclerosus. Three months after the completion of treatment, the laser treatment group showed no statistically significant difference between PGI-C scores for the 2 pathological subtypes (P>0.05). However, the efficacy index indicated that the proportion of patients with lichen simplex chronicus who improved after treatment (improvement rate) was 80.00% (16/20), which was superior to that of patients with lichen sclerosus [50.00% (10/20)]. For the laser treatment group, for the 2 pathologic subtypes, patients with lichen simplex chronicus significantly improved 6 months (P=0.006) and 12 months (P=0.024) after the completion of treatment, and the improvement rate for patients with lichen simplex chronicus reached 80.00% (16/20); the improvement rate for patients with lichen sclerosus was only 30.00% (6/20). In the electrostimulation group, the PGI-C scores were significantly different between patients with lichen simplex chronicus and patients with lichen sclerosus 3 months (P=0.001) and 12 months (P=0.021) after the completion of treatment. The subjective improvement of patients with lichen simplex chronicus was higher than that of patients with lichen sclerosus (Table 5).
Table 5
| Efficacy score | PGI-C | Significantly improved | Improved | Slightly improved | Unimproved | Total | P |
|---|---|---|---|---|---|---|---|
| 3 months after completion of treatment | |||||||
| Electrostimulation group | Lichen simplex chronicus | 12 | 3 | 5 | 0 | 20 | 0.001 |
| Lichen sclerosus | 2 | 9 | 4 | 5 | 20 | ||
| Laser treatment group | Lichen simplex chronicus | 16 | 2 | 2 | 0 | 20 | 0.156 |
| Lichen sclerosus | 10 | 7 | 2 | 1 | 20 | ||
| 6 months after completion of the treatment | |||||||
| Electrostimulation group | Lichen simplex chronicus | 8 | 6 | 4 | 2 | 20 | 0.098 |
| Lichen sclerosus | 4 | 2 | 8 | 6 | 20 | ||
| Laser treatment group | Lichen simplex chronicus | 16 | 3 | 1 | 0 | 20 | 0.006 |
| Lichen sclerosus | 6 | 9 | 4 | 1 | 20 | ||
| 12 months after completion of treatment | |||||||
| Electrostimulation group | Lichen simplex chronicus | 8 | 7 | 3 | 2 | 20 | 0.021 |
| Lichen sclerosus | 2 | 3 | 9 | 6 | 20 | ||
| Laser treatment group | Lichen simplex chronicus | 14 | 4 | 1 | 1 | 20 | 0.024 |
| Lichen sclerosus | 6 | 10 | 4 | 0 | 20 | ||
PGI-C, Patient Global Impression of Change.
Comparison of clinical efficacy scores
From the clinical efficacy scores of the 2 groups 3 months after the completion of treatment, the therapeutic efficacies for the 2 pathological subtypes in the electrostimulation group were significantly different (P<0.05), and the clinical efficacy for lichen simplex chronicus was higher than that for lichen sclerosus in the electrostimulation group (95.00% vs. 60.00%). In the electrostimulation group, the clinical efficacy for lichen simplex chronicus was significantly higher than that for lichen sclerosus 6 months (95.00% vs. 60.00%, P=0.019) and 12 months (95.00% vs. 40.00%, P=0.000) after the completion of treatment. In the laser treatment group, the clinical efficacies for the 2 pathological subtypes were nonsignificant (100% vs. 80.00%, P>0.05) 3 months after the completion of treatment, proving that laser treatment is effective for both pathological types. The clinical efficacies for the 2 pathological subtypes in the laser treatment group were significantly different 6 months (P=0.047) and 12 months (P=0.047) after the completion of treatment, and the clinical efficacy for lichen simplex chronicus was significantly higher than that for lichen sclerosus 6 months (95.00% vs. 75.00%) and 12 months (95.00% vs. 70.00%) after the completion of treatment (Table 6).
Table 6
| Grouping | Classification | Cured | Effective | Ineffective | Total effective rate | Total | P |
|---|---|---|---|---|---|---|---|
| 3 months after completion of treatment | |||||||
| Electrostimulation group | Lichen simplex chronicus | 1 | 18 | 1 | 95.00% | 20 | 0.019 |
| Lichen sclerosus | 0 | 12 | 8 | 60.00% | 20 | ||
| Laser treatment group | Lichen simplex chronicus | 1 | 19 | 0 | 100.00% | 20 | 0.106 |
| Lichen sclerosus | 1 | 15 | 4 | 80.00% | 20 | ||
| 6 months after completion of treatment | |||||||
| Electrostimulation group | Lichen simplex chronicus | 1 | 18 | 1 | 95.00% | 20 | 0.019 |
| Lichen sclerosus | 0 | 12 | 8 | 60.00% | 20 | ||
| Laser treatment group | Lichen simplex chronicus | 1 | 18 | 1 | 95.00% | 20 | 0.047 |
| Lichen sclerosus | 1 | 14 | 5 | 75.00% | 20 | ||
| 12 months after completion of treatment | |||||||
| Electrostimulation group | Lichen simplex chronicus | 1 | 18 | 1 | 95.00% | 20 | 0.000 |
| Lichen sclerosus | 0 | 8 | 12 | 40.00% | 20 | ||
| Laser treatment group | Lichen simplex chronicus | 1 | 18 | 1 | 95.00% | 20 | 0.047 |
| Lichen sclerosus | 0 | 14 | 6 | 70.00% | 20 | ||
Discussion
This study used 2 different methods, fractional Carbon Dioxidelaser and electrostimulation of smooth muscle, to treat non-neoplastic epithelial disorders of the vulva and compared their clinical efficacies. The PGI-C scores showed that 3, 6 and 12 months after the completion of treatment, subjective improvement in the laser treatment group was better than that in the electrostimulation group. This result is in agreement with the results reported by Lee et al. and Stuart et al. Lee et al. performed fractional Carbon Dioxidelaser therapy on 4 patients with vulvar lichen sclerosus, for whom corticosteroid treatments were ineffective, and the subjective symptoms improved in all 4 patients after treatment. In addition, they found that Carbon Dioxide is very effective in inhibiting hyperkeratosis in clinical practice (7). Stuart et al. reported that 6 out of 7 patients with vulvar lichen sclerosus, who did not respond to other treatments, were asymptomatic after laser ablation (8). In 2011, Gaspar et al. reported a controlled study of 40 cases of non-neoplastic epithelial disorders of the vulva treated by fractional Carbon Dioxide laser. The results showed that symptoms such as pruritus vulvae and intercourse pain were significantly mitigated, and no adverse events occurred (9). This may be related to the thermal effect of the laser, which causes tissue oedema and the release heat-shock protein 70 and transforming growth factors and promotes fibroblast proliferation and the synthesis of extracellular matrices such as collagen and proteoglycan, thereby restoring tissue elasticity, initiating vascular reconstruction and increasing blood flow (10). As a result, the blood supply to and nutrition for the skin improved in the 2 lichen-like lesions of the vulva, the local scratched and damaged tissues were repaired, the integrity and elasticity of the vulvar skin were maintained, and local resistance to the outside environment was enhanced. Our study also showed that the total effective rates for both treatment regimens were more than 50.00%, 3, 6, and 12 months after the completion of treatment; in the laser treatment group, clinical efficacy was most pronounced and was stable for a long period, and the total effective rate reached 90.00% 3 months after the completion of treatment and stabilized at 85.00% 6 and 12 months after the completion of treatment. This result is similar to that reported by Peterson et al. (11), who found that patients with vulvar lichen sclerosus treated with Carbon Dioxide laser had normal epithelium in regenerated vulvar tissue and that if no further treatment was provided, the symptoms lasted longer (2–3 years).
This study also showed that electrostimulation also had a good effect in the treatment of non-neoplastic epithelial disorders of the vulva, which may be related to the pathogenic mechanism of non-neoplastic epithelial disorders of the vulva. Studies have shown that the major ultrastructural changes in non-neoplastic epithelial disorders of the vulva are characterized by the narrowing and stenosis of intradermal capillary lumens, the widening of gaps between cells, and the reduction in desmosomes and melanin granules (12). The low resistance caused by microcirculatory disorders that are triggered by cellular energy and material metabolism disorders may result in secondary local inflammation, while inflammatory mediators stimulate the peripheral nerves to cause pruritus vulvae and repeated scratching further aggravates skin lesions, thus forming a vicious cycle (13,14). Electrostimulation of vascular smooth muscle can electrically stimulate vascular smooth muscle, improve the local microcirculation of vulvar skin, local vulvar lymph circulation reflux, local microcirculation and microenvironment, and tissue repair ability, thereby restoring the immune function of the vulva, improving hormone receptors and sensitivity, and further improving the symptoms and physical signs of patients with lichen simplex chronicus and lichen sclerosus.
More importantly, the results of this study showed that different pathological types showed different responses to different therapeutic methods. Whether subjective improvement or clinical efficacy was compared, lichen simplex chronicus showed a better response to both electrostimulation and laser treatment than did lichen sclerosus, indicating that the pathogenesis and molecular biology of lichen simplex chronicus and lichen sclerosus may be different (15). However, causes for different treatment responses of different pathological types may require further investigation.
This study has the following limitations. (I) Although compared with existing reports the sample size of our study was not too small, a larger sample size could better reduce the selectivity bias. (II) A multicentre randomized controlled study is needed to provide better evidence for clinical treatment decision-making. (III) A longer follow-up time could further validate the long-term efficacy of different therapeutic methods.
In summary, compared with electrostimulation, fractional Carbon Dioxidelaser treatment resulted in better PGI-C scores and clinical efficacy and better long-term stability in patients with non-neoplastic epithelial disorders of the vulva. In addition, for different pathological subtypes of non-neoplastic epithelial disorders of the vulva, the treatment efficacy for lichen simplex chronicus was higher than that for lichen sclerosus. Therefore, for patients with poor response to electrostimulation, fractional Carbon Dioxidelaser treatment can be used as a new therapeutic option for non-neoplastic epithelial disorders of the vulva.
Acknowledgments
Funding: This study was funded by the foundation of Science & Technology Department of Sichuan Province (Nos. 2019YJ0044, 16H0864) and the foundation of Chinese Preventive Medicine Association special prevention and treatment of pelvic floor dysfunction (No. 201822163).
Footnote
Reporting Checklist: The authors have completed the STROBE reporting checklist. Available at https://gpm.amegroups.com/article/view/10.21037/gpm-20-40/rc
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://gpm.amegroups.com/article/view/10.21037/gpm-20-40/coif). XN serves as an Editor-in-Chief of Gynecology and Pelvic Medicine. The other authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. This study was approved by the ethics committee at West China Second University Hospital, Sichuan University (registration number: 2019YJ0044), and all experiments were performed in accordance with relevant guidelines and regulations. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). All patients voluntarily participated in the study and signed an informed consent for clinical studies.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- McCluggage WG. Recent developments in vulvovaginal pathology. Histopathology 2009;54:156-73. [Crossref] [PubMed]
- Markowska J, Madry R, Markowska A. The effect of hyaluronic acid (Cicatridine) on healing and regeneration of the uterine cervix and vagina and vulvar dystrophy therapy. Eur J Gynaecol Oncol 2011;32:65-8. [PubMed]
- Mezzana P, Valeriani M, Valeriani R. Combined fractional resurfacing (10600 nm/1540 nm): Tridimensional imaging evaluation of a new device for skin rejuvenation. J Cosmet Laser Ther 2016;18:397-402. [Crossref] [PubMed]
- Geisser ME, Clauw DJ, Strand V, et al. Contributions of change in clinical status parameters to Patient Global Impression of Change (PGIC) scores among persons with fibromyalgia treated with milnacipran. Pain 2010;149:373-8. [Crossref] [PubMed]
- Cattaneo A, Bracco GL, Maestrini G, et al. Lichen sclerosus and squamous hyperplasia of the vulva. A clinical study of medical treatment. J Reprod Med 1991;36:301-5. [PubMed]
- Li C, Bian D, Chen W, et al. Focused ultrasound therapy of vulvar dystrophies: a feasibility study. Obstet Gynecol 2004;104:915-21. [Crossref] [PubMed]
- Lee A, Lim A, Fischer G. Fractional carbon dioxide laser in recalcitrant vulval lichen sclerosus. Australas J Dermatol 2016;57:39-43. [Crossref] [PubMed]
- Stuart GC, Nation JG, Malliah VS, et al. Laser therapy of vulvar lichen sclerosus et atrophicus. Can J Surg 1991;34:469-70. [PubMed]
- Gaspar A, Addamo G, Brandi H. Vaginal Fractional CO2 Laser: A Minimally Invasive Option for Vaginal Rejuvenation. The American Journal of Cosmetic Surgery 2011;28:156-62. [Crossref]
- Perino A, Calligaro A, Forlani F, et al. Vulvo-vaginal atrophy: a new treatment modality using thermo-ablative fractional CO2 laser. Maturitas 2015;80:296-301. [Crossref] [PubMed]
- Peterson CM, Lane JE, Ratz JL. Successful carbon dioxide laser therapy for refractory anogenital lichen sclerosus. Dermatol Surg 2004;30:1148-51. [PubMed]
- Carlson BC, Hofer MD, Ballek N, et al. Protein markers of malignant potential in penile and vulvar lichen sclerosus. J Urol 2013;190:399-406. [Crossref] [PubMed]
- Liu X, Li J, Li L, et al. Expression of VEGF and MVD in Nonneoplastic Epithelial Disorders of Vulva, VIN and Vulvar Squamous Carcinoma. Chinese Journal of Laboratory Diagnosis 2011;15:1334-6.
- Chen Y, Li K, Zhang L, et al. Expression and clinical significance of CD34 in white lesions of the vulva. Maternal & Child Health Care of China 2013;28:133-5.
- Simpkin S, Oakley A. Clinical review of 202 patients with vulval lichen sclerosus: A possible association with psoriasis. Australas J Dermatol 2007;48:28-31. [Crossref] [PubMed]
Cite this article as: Wei D, Chen Y, Yang J, Hu Y, Niu X. Prospective cohort study of the treatment of non-neoplastic epithelial disorders of the vulva with a fractional Carbon Dioxide laser. Gynecol Pelvic Med 2022;5:17.



