
Unusual presentation of hemoperitoneum secondary to ruptured uterine leiomyoma: a case report
Introduction
Uterine fibroids or leiomyomas are the most common benign tumours affecting women of reproductive age. They arise from the smooth muscle cells of the myometrium (1). Certain factors increase the likelihood of development of a leiomyoma including increased oestrogen exposure, obesity, hypertension, diet high in red meat, hypertension, age between 30–40 years old and ethnic or genetic susceptibility (2).
Uterine fibroids can cause pain, dysfunctional uterine bleeding as well as infertility. Complications of leiomyomas include torsion, red degeneration, carcinomatous change and rarely—perforation and/or haemorrhage (3).
The usual presentation of haemorrhage from a uterine fibroid is of sudden and profound hypovolemic shock with severe abdominal pain. Preoperative imaging is not reliable at making the correct diagnosis and the diagnosis is often made post mortem (3-5).
Management can usually be conservative; however, it can also be managed medically with progesterone and GnRH agonists. Surgical management includes hysteroscopic, laparoscopic or open myomectomy, or with thermal ablation or uterine artery embolization.
We present a case report where the presentation is atypical—our patient remained haemodynamically stable and we were able to consider and investigate all possible differential diagnosis prior to operative management. Our patient’s presenting symptoms and preoperative course can guide other clinicians to consider a spontaneous hemorrhage from a uterine fibroid as a differential of hemoperitoneum and subsequently expedite definitive management. We present the following case in accordance with the CARE reporting checklist (available at https://gpm.amegroups.com/article/view/10.21037/gpm-21-54/rc).
Case presentation
We report a case of an atypical presentation of spontaneous hemorrhage from a large uterine fibroid with no precipitating factors in a stable patient who did not require blood transfusion. A timeline is attached for ease of interpretation (Figure 1).
A 28-year-old nulliparous woman presented on 17/12/20 at 05:00 with a 2-day history of worsening lower abdominal pain and an outpatient pelvic ultrasound (US) suggesting hemoperitoneum.
The pain started 2 days prior (from 15/12/20) in the suprapubic region then migrated upwards. It was exacerbated by mobilisation, urination with associated dysuria.
She had no precipitating illnesses, no other symptoms, no nausea, vomiting, diarrhoea or any recent abdominal trauma or injury.
In terms of her obstetric and gynecology history—she was sexually active and was in a long-term monogamous relationship but had not been sexually active in the last 9 months. She had one previous miscarriage. She had regular 28/5-day menstrual cycles and was on day 10 of her cycle. She denied any past medical history and took no regular medications. She was a non-smoker.
On examination she was hemodynamically stable—blood pressure: 109/75; heart rate: 84; respiratory rate: 18. She appeared comfortable and had warm, well perfused peripheries. Her abdomen was soft, generally tender across the lower abdomen with some voluntary guarding. There was no peritonism and no obvious masses. Her body mass index was 19.
Her initial blood tests at 17/12/21 10:30 showed a Hb of 114 g/L (normal range, 115–165 g/L) and leucocytosis 13.7×109/L (normal range, 3.9×109/L–11.1×109/L). Her lactate was 2.1 mmol/L (normal range, ≤2.0 mmol/L) on a venous blood gas sample. She had an urgent US on 17/12/20 13:10 reporting a large vascular complex pelvic mass of uncertain etiology with a large amount of hemoperitoneum (at least 430 mL) with further complex fluid, likely blood surrounding the liver and spleen (Figure 2).
She was reviewed by the general surgeons whose opinion was that this was most likely of gynecological etiology.
An urgent computed tomography (CT) abdomen/pelvis (Figure 3) on 17/12/20 16:24 demonstrated extensive hemoperitoneum, but no active arterial blush of contrast extravasation was seen. A large 86×94 mm exophytic homogenously enhancing mass lesion was seen in the centre of the pelvis which appeared to arise from the posterior aspect of the uterus and pushing the cervix and the urinary bladder anteriorly. It had prominent vascular nets mainly supplied by the right uterine artery with a small central hypodensity suggestive of possible necrosis/cystic degeneration. There was effacement of the urinary bladder from mass effect of enlarged uterus and hemoperitoneum, with associated minor to moderate bilateral hydronephrosis.
A second opinion was obtained from gyne-oncology due to the unusual presentation and large pelvic mass—there was significant clinical suspicion that the presentation was as a result of a malignant process. Given the patient was stable, it was recommended for magnetic resonance imaging (MRI) pelvis to further delineate the mass for surgical planning as well as repeat blood tests to assess the progress.
MRI pelvis on 17/12/20 20:05 showed a central pelvic mass measuring 9.7 cm × 8.8 cm × 7.3 cm [antero-posterior (AP) × transverse (TV) × superior to inferior (SI)] outside the uterus, with mild central cystic changes (Figure 4A,4B). The interface between the mass and the uterine fundus was ill-defined. Possible differentials included a pedunculated uterine mass, leiomyoma, leiomyosarcoma, and other forms of pelvic mesenchymal tumour/sarcoma.
Serial Hb levels showed an initial drop to 86 g/L on 17/12/20 21:40 (normal range, 115–165 g/L) (from 114 g/L) 12 hours after presentation, which stabilized to 89 g/L 38 hours later on 18/12/20 20:16.
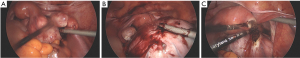
Given these findings the main differential diagnosis was of a pelvic malignancy with complication causing hemoperitoneum. The patient underwent urgent diagnostic laparoscopy under the care of the gyne-oncologist on 18/12/20 11:00. Direct entry at the umbilicus was performed with a 10 mm port; 3×5 mm accessory ports were inserted. A large pedunculated fibroid arising from right anterior cornua found with approximately 1 L hemoperitoneum (Figure 5A). An active bleeding point was identified arising from the fibroid (Figure 5B). The uterus, bilateral ovaries and fallopian tubes appeared unremarkable. Given the findings, lack of pre-procedure counselling regarding morcellation and with some difficulty in controlling the bleeding with energy devices, we proceeded to laparotomy. The fibroid pedicle was secured with LigaSure and the fibroid detached (Figure 5C). The specimen was removed en bloc through a Pfannenstiel incision. Continuous 1.0 Vicryl, non-locking sutures was applied to base of fibroid on anterior cornua with overlying Surgicel.
Postoperatively her Hb remained stable—80 g/L (19/12/20 06:45), and she was discharged day 2 post operatively on 20/12/20 09:00. The histopathology showed leiomyoma measuring 90×80×60 mm weighing 305 g with infarction necrosis. She was well at the 6-week postoperative follow-up, the wound had healed well. There were no adverse events to report at this follow-up.
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the editorial office of this journal. Ethics approval has been granted by the Western Sydney Local Health District Human Research and Ethics Committee.
Discussion
Intraperitoneal hemorrhage associated with bleeding from either the rupture of a surface vessel of a subserosal leiomyoma or spontaneous haemorrhage is a life-threatening and rare complication with 125 cases reported in literature thus far with 4 fatalities (4,5). In most cases bleeding from a uterine leiomyoma was associated with rupture of superficial blood vessels over the surface of a fibroid followed by rupture or avulsion of a fibroid (5). In most cases, the source vessel was mainly venous in origin (6).
Suggested theories for the pathophysiology of the rupture of the vessels include large fibroids overstretching superficial vessels resulting in rupture. Increased intra-abdominal pressure and venous congestion in cases such as menstruation, pregnancy, strenuous exercise, weight-bearing exercises can cause passive venous congestion and subsequent rupture of superficial vessels overlying the fibroid (7,8). There were no superficial vessels (ruptured or otherwise) seen at laparoscopy for our patient but instead a bleeding point was identified on the fibroid—suggesting that the rupture was a rare spontaneous event.
The usual presentation of hemorrhage secondary to uterine fibroids is of a patient with severe, sharp pain with sudden and profound hypovolaemic shock (5). We present a case of an unusual presentation, compared to the typical, for intra-abdominal hemorrhage secondary to uterine fibroids. Our patient remained stable and although she had a hemoperitoneum of 1 L with ongoing bleeding, she did not require blood transfusion and was able to be discharged day one post-operatively.
Imaging
Intra-abdominal hemorrhage secondary to uterine fibroids is a rare phenomenon which is often misdiagnosed. In the review by Lim et al. (5) only 7 of the 125 cases had a correct pre-operatively diagnosis made on CT. This case highlights the importance of consideration of rare differentials, such as hemorrhage. We had considered the likelihood of hemorrhage from a uterine fibroid to be remote and proceeded with further imaging through CT, MRI as well as a gynae-oncology consult rather than proceeding directly to laparoscopy which could have compromised the patient’s care.
Pelvic US and MRI have no role in definite diagnosis in this scenario and CT imaging with arterial contrast is the best diagnostic modality (5). US is safe, cheap and readily accessible and can be performed readily as a first-line investigation. Contrast enhanced CT can also be performed as a rapid and sensitive exam to identify pelvic and abdominal etiologies of hemoperitoneum and an acute abdomen (3). MRI can be useful in further delineating the nature of the diagnosis as well but is not suitable in cases of emergency. In the 125 cases identified by Lim et al. (5) only 2 patients had a MRI performed.
Management
Adequate resuscitation of the patient is paramount. If the patient is stable, imaging could be considered to delineate a possible etiology. Surgical management is definitive and recommended in any case of an unstable patient with evidence of hemoperitoneum.
Management options for leiomyoma haemorrhage include laparoscopy, laparotomy, myomectomy, hysterectomy as well as interventional radiology guided uterine artery embolization. In the literature, cases of hemorrhage from a uterine fibroid have been managed with myomectomy, hysterectomy, and embolization of uterine arteries (9).
Only two cases of hemorrhage secondary to a uterine fibroid have been managed successfully with laparoscopy. In our case the procedure could have proceeded via laparoscopy however primarily due to the concerns regarding possible dissemination of malignancy, laparotomy was performed to retrieve the specimen en bloc. If the patient has been adequately counselled and consented preoperatively it would be appropriate to manage these patients laparoscopically with morcellation.
The strength of this case report lies in its comprehensive assessment of the patient’s presentation and consideration of differential diagnosis as well as follow-through of the patient’s management to postoperative follow-up. The findings contribute to the small body of literature describing rare complications of uterine fibroids and report a very unusual presentation of a ruptured fibroid that clinicians can consider for their own patients. The limitations include the use of multiple modalities of imaging that may not be available in all health care settings and therefore can limit the usefulness of recommendations for investigations. Management options may also be limited by resources and not reproducible in all settings.
An acute and severe presentation of intra-abdominal haemorrhage in women of reproductive age is usually attributed to a ruptured ectopic pregnancy, ruptured corpus luteum or adnexal accident. Hemorrhage secondary to a uterine fibroid is a rare complication of uterine fibroids that clinicians must consider without reducing vigilance for other intra-abdominal causes of haemorrhage. Consideration of this rare complication as a differential diagnosis when presented with an acute intra-abdominal haemorrhage and pelvic mass can assist clinicians with patient counselling as well as rapid and definitive management in a minimally invasive way.
Initial rapid imaging via US or more reliably CT with arterial contrast can be used to narrow down the diagnosis. Prompt resuscitation, definitive surgical management in a multi-disciplinary team approach will aid in management and improve outcomes.
Acknowledgments
Funding: None.
Footnote
Reporting Checklist: The authors have completed the CARE reporting checklist. Available at https://gpm.amegroups.com/article/view/10.21037/gpm-21-54/rc
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://gpm.amegroups.com/article/view/10.21037/gpm-21-54/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the editorial office of this journal. Ethics approval has been granted by the Western Sydney Local Health District Human Research and Ethics Committee.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Murase E, Siegelman ES, Outwater EK, et al. Uterine leiomyomas: histopathologic features, MR imaging findings, differential diagnosis, and treatment. Radiographics 1999;19:1179-97. [Crossref] [PubMed]
- Roche O, Chavan N, Aquilina J, et al. Radiological appearances of gynaecological emergencies. Insights Imaging 2012;3:265-75. [Crossref] [PubMed]
- Mizrahi DJ, Kaushik C, Adamo R. Hypovolemic Shock and Hemoperitoneum from Spontaneous Avulsion of a Large Pedunculated Uterine Leiomyoma. J Radiol Case Rep 2017;11:15-21. [Crossref] [PubMed]
- Ihama Y, Miyazaki T, Fuke C. Hemoperitoneum due to rupture of a subserosal vein overlying a uterine leiomyoma. Am J Forensic Med Pathol 2008;29:177-80. [Crossref] [PubMed]
- Lim WH, Cohen SC, Lamaro VP. Intra-abdominal haemorrhage from uterine fibroids: a systematic review of the literature. BMC Surg 2020;20:70. [Crossref] [PubMed]
- Althobaiti FA, Alsaadi KK, Althobaiti AA. A Case of Hemoperitoneum Due to Spontaneous Bleeding from a Uterine Leiomyoma. Am J Case Rep 2019;20:167-70. [Crossref] [PubMed]
- Fontarensky M, Cassagnes L, Bouchet P, et al. Acute complications of benign uterine leiomyomas: treatment of intraperitoneal haemorrhage by embolisation of the uterine arteries. Diagn Interv Imaging 2013;94:885-90. [Crossref] [PubMed]
- Gulati N, Raman S, Srinivasan M, et al. Rare gynaecological emergency: massive intraperitoneal haemorrhage from spontaneous rupture of a superficial vessel on a large leiomyoma. BMJ Case Rep 2016;2016:bcr2015212576. [Crossref] [PubMed]
- Levai AM, Rotar IC, Muresan D. Torsion of a uterine leiomyoma - a rare cause of hemoperitoneum; a case report and review of the literature. Med Ultrason 2019;21:77-82. [Crossref] [PubMed]
Cite this article as: Hu H, Choi JDW, Arrage N. Unusual presentation of hemoperitoneum secondary to ruptured uterine leiomyoma: a case report. Gynecol Pelvic Med 2022;5:19.






